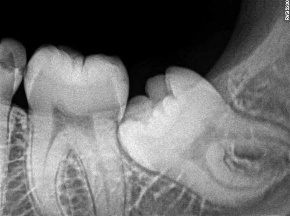
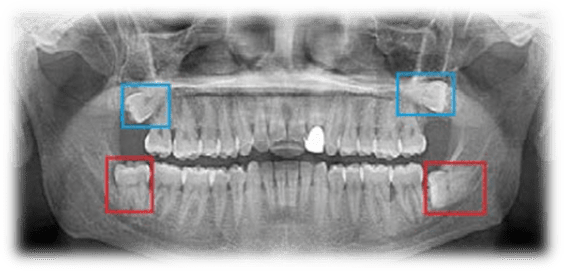
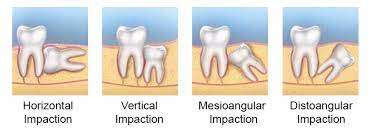
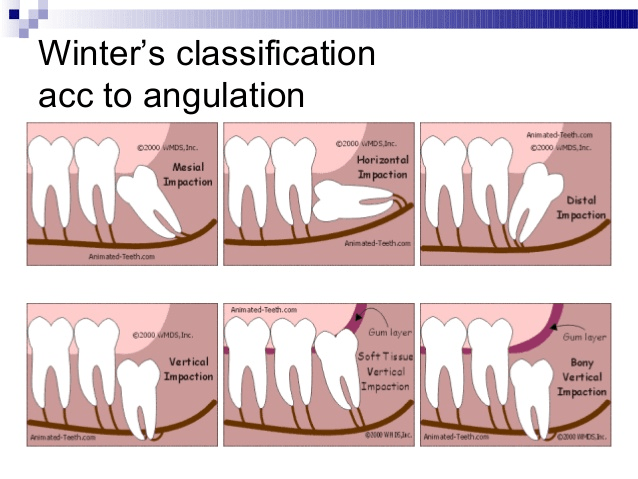
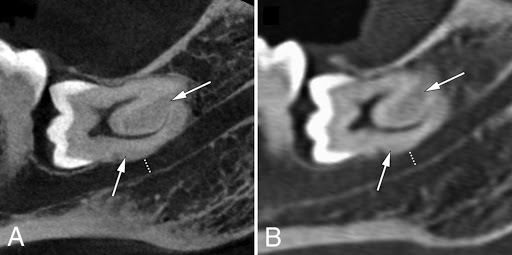
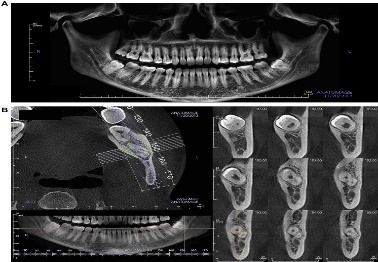
Wisdom teeth, otherwise known as third molars, are the last set of teeth to develop. Sometimes these teeth emerge from the gum line and the jaw is large enough to allow room for them. However, most of the time, this is not the case. More often, one (or more) of these third molars fails to emerge in proper alignment or fully through the gum line and becomes entrapped or “impacted” between the jawbone and the gum tissue.