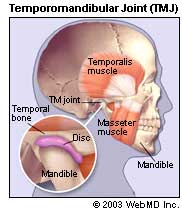
Your Temporomandibular joint is a hinge that connects your jaw to the temporal bones of your skull, which are in front of each ear. It lets you move your jaw up and down and side to side, so you can talk, chew, and yawn.
There is also a cartilage disc within the joint. The joint is lubricated by fluid called synovial fluid.
Problems with your jaw, the muscles in your face that control the joint, as well as internal components of the joint, are collectively known as temporomandibular disorders (TMD). But you may hear it wrongly called TMJ, after the joint.
It is believed that the symptoms arise from problems with the muscles of your jaw or with the parts of the joint itself. Injury or undue stress to your jaw, the joint, or the muscles of your head and neck can lead to TMD. Other causes include:
Common symptoms include:
FMS has an exclusive department for the diagnosis and management of the TMJ disorders.
The diagnosis involves
(FMS has established the first TMD center in the state)
How to manage TM Joint disorders ?
The management of the TMJ disorders depends on the diagnosis and severity of the problem.
Mild cases it can be managed with home care combined with medication
Till you go to see the TMJ Specialist, they will guide with lifestyle changes
Moderate TM Joint disorders
Your dentist can prescribe appropriate NSAIDs & Muscle Relaxants
Severe cases of TM Joint disorders
Surgery for TMD
If other treatments can’t help you, or in very severe cases surgery is required. There are three types of surgery for TMD. The type you need depends on the problem.
What is the Prognosis for TMJ disorders?
Generally the outlook is good. Most TMJ disorders improve over time with appropriate treatment. It is very rare to get any complications with this condition. Some people do have symptoms that last longer or recur, but even these can usually be improved with the treatments described above.