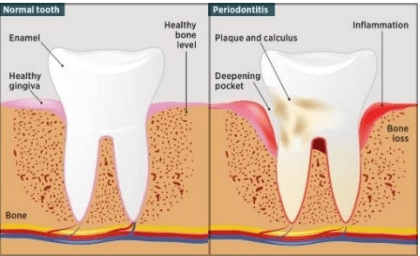
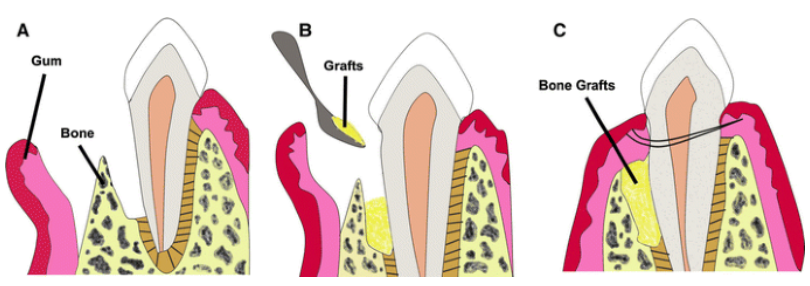
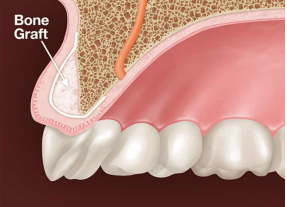
Teeth are held intact by gums, bone, and other tissues, however gum diseases can cause the bone to break down and regenerative procedures can be used to stimulate growth of new bone, this gives the tooth more support. It increases the amount of attachment around the root of the tooth. Restoring even half of the amount of lost bone extends the life of the tooth. Among the many procedures available to accomplish this task are bone grafts, PRF and guided tissue regeneration (GTR).