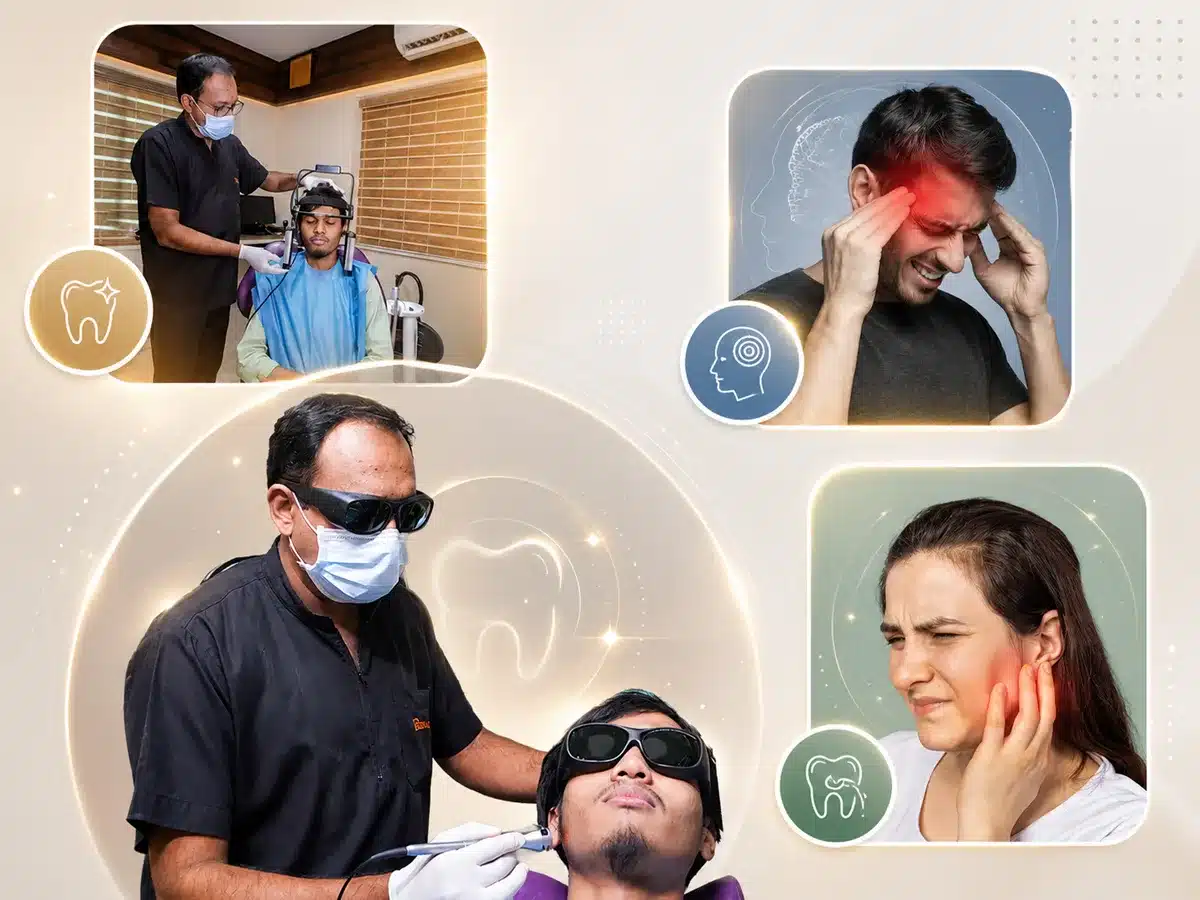
Why Do I Keep Getting Headaches Along with Jaw Pain?
If your headaches are frequently accompanied by jaw stiffness, facial tension, ear discomfort, or clicking sounds while chewing, the underlying cause may not actually be neurological – it could be related to the jaw joint itself.
For many people, these symptoms appear unrelated. But in reality, they are often connected to one commonly overlooked condition: Temporomandibular Disorder (TMD).
Because the jaw joint shares close muscular and nerve connections with the temples, ears, neck, and face, TMJ dysfunction can often create pain that radiates well beyond the jaw.
At FMS Dental, TMJ specialist Dr. Faisal Zardi and the neuromuscular dentistry team regularly see patients who have spent months – sometimes years – treating headaches, sinus pressure, ear discomfort, or facial pain without realizing the actual source may be the jaw joint itself.
The encouraging part is that most TMJ disorders can be treated successfully without surgery when diagnosed early and accurately.
What Exactly Is the TMJ – And What Is TMD?
The Temporomandibular Joint (TMJ) is the joint connecting your lower jaw (mandible) to the skull, located just in front of the ears on both sides of the face.
This joint is responsible for nearly every jaw movement you make:
- chewing
- speaking
- swallowing
- yawning
- smiling
Unlike most joints in the body, the TMJ performs both hinge and sliding movements simultaneously. That complexity is one reason TMJ problems can affect far more than just the jaw itself.
When the joint, muscles, nerves, and bite alignment stop functioning harmoniously, it can lead to Temporomandibular Disorder (TMD) – a condition that may involve:
- jaw pain
- headaches
- muscle tension
- ear symptoms
- restricted jaw movement
- bite imbalance
How TMJ Dysfunction Affects Different Structures
| Structure Affected | What Happens | Common Symptom |
| Articular disc | Cushioning disc shifts position | Clicking or popping |
| Jaw muscles | Muscles become overworked | Facial soreness |
| Trigeminal nerve system | Pain signals spread widely | Headaches, ear pain |
| Bite alignment | Uneven bite causes compensation | Tooth wear, jaw fatigue |
| Neck muscles | Tension radiates downward | Neck stiffness |
Many patients are surprised to learn that the problem is not always the joint alone. In fact, muscular imbalance and bite-related strain are often major contributors to chronic TMD symptoms.
Can TMJ Problems Really Cause Headaches, Ear Pain, and Neck Stiffness?
Yes — and this is one of the most commonly overlooked aspects of TMD.
The jaw joint shares close connections with:
- facial muscles
- neck muscles
- trigeminal nerves
- ear structures
As a result, TMJ dysfunction can produce symptoms that mimic:
- migraines
- sinus headaches
- ear infections
- tension headaches
Many patients are surprised to discover that their chronic headaches or ear pressure may actually originate from overworked jaw muscles, night-time grinding, or bite imbalance.
Common Warning Signs of TMD
- Morning headaches
- Jaw clicking or popping
- Pain while chewing
- Ringing in the ears (tinnitus)
- Facial tightness or soreness
- Neck pain associated with jaw movement
- Difficulty opening the mouth fully
- Jaw locking episodes
- Teeth grinding during sleep
At FMS Dental, it is common to see patients who first visit neurologists or ENT specialists before eventually discovering that the underlying issue is jaw dysfunction.
“One patient who visited FMS Dental had been undergoing migraine treatment for nearly two years before a detailed TMJ evaluation revealed severe night-time clenching and bite imbalance. After neuromuscular splint therapy and muscle rehabilitation, both the jaw discomfort and headache frequency improved significantly.”
Why Neuromuscular Dentistry Matters in TMJ Treatment
One of the biggest reasons TMJ disorders are often misunderstood is because traditional treatment may focus only on the teeth or pain symptoms – not on the entire jaw-muscle-joint relationship.
At FMS Dental, TMJ treatment is based on the principles of Neuromuscular Dentistry – an advanced approach that evaluates how the:
- jaw joints
- facial muscles
- teeth
- bite alignment
- nerves
- airway
- head and neck posture
All function together as one interconnected system.
This approach remains relatively uncommon in many dental practices, which is why patients with chronic TMJ symptoms are frequently misdiagnosed or treated only symptomatically.
Unlike conventional dentistry, neuromuscular dentistry aims to identify the jaw’s ideal physiological position — where:
- the muscles are relaxed
- the joints are stable
- the bite functions without excessive strain
This becomes especially important because many TMJ patients may appear to have a “normal bite,” while hidden muscular imbalance continues causing:
- headaches
- teeth grinding
- facial pain
- jaw locking
- neck stiffness
- ear symptoms
By identifying these hidden imbalances, neuromuscular dentistry helps address the root cause of TMD rather than simply masking symptoms temporarily.
What Causes TMD?
TMD rarely develops because of a single issue. Most cases involve multiple contributing factors that gradually overload the jaw joint and surrounding muscles over time.
| Cause | How It Contributes to TMD |
| Teeth grinding (Bruxism) | Places excessive pressure on jaw muscles and joints |
| Bite imbalance | Forces muscles to compensate continuously |
| Stress & anxiety | Increases clenching and muscle tension |
| Trauma or injury | Damages joint structures |
| Arthritis | Causes inflammation inside the joint |
| Poor posture | Alters jaw and neck mechanics |
| Missing teeth | Changes bite stability |
How Is TMD Diagnosed?
Accurate diagnosis is the foundation of effective TMJ treatment.
At FMS Dental, diagnosis involves far more than simply checking for jaw pain. The goal is to determine whether the primary issue is:
- muscular
- joint-related
- bite-related
- or a combination of all three
Many patients are surprised by how detailed a comprehensive TMJ evaluation actually is.
Advanced Neuromuscular Technologies Used at FMS Dental
| Technology | Purpose |
| T-Scan Digital Analysis | Maps bite force distribution |
| EMG (Electromyography) | Measures muscle activity |
| 3D Jaw Tracking | Evaluates jaw movement |
| BioJVA | Detects joint vibration abnormalities |
| CBCT Imaging | Provides detailed 3D joint analysis |
| TENS Therapy | Relaxes muscles before evaluation |
These technologies help identify:
- muscle hyperactivity
- joint instability
- disc displacement
- premature bite contacts
- functional bite imbalance
This detailed neuromuscular approach is one of the reasons FMS Dental stands out in advanced TMJ care.
What Dental Treatments Actually Help TMJ Headaches and Jaw Pain?
TMJ treatment depends entirely on the underlying cause. The goal is not simply pain relief – but restoring harmony between the jaw joints, muscles, teeth, and nerves.
The encouraging part is that most patients improve successfully with non-surgical treatment.
1. Neuromuscular Splints / Occlusal Splints
Custom-designed splints help:
- reduce grinding pressure
- relax overactive muscles
- protect teeth from wear
- improve jaw stability
- reduce headaches
Unlike over-the-counter mouth guards, neuromuscular splints are designed using digital jaw analysis for precision.
2. TENS Therapy
TENS (Transcutaneous Electrical Nerve Stimulation) uses low-frequency electrical pulses to relax hyperactive jaw and neck muscles.
Benefits may include:
- reduced muscle spasms
- better jaw comfort
- decreased facial tension
- improved bite analysis accuracy
Many patients feel noticeable muscle relaxation even during the first session.
3. Low-Level Laser Therapy (LLLT)
Low-level laser therapy helps:
- reduce inflammation
- improve tissue healing
- relieve joint discomfort
- improve mobility
This treatment is completely non-invasive and particularly useful for inflamed joints and chronic pain.
4. Bite Correction and Occlusal Balancing
If bite imbalance contributes to TMD, treatment may involve:
- bite adjustments
- orthodontic treatment
- replacing faulty restorations
- restoring missing teeth
- full-mouth rehabilitation
Correcting uneven bite forces can significantly reduce long-term muscular overload.
5. Physiotherapy and Rehabilitation
Some TMJ disorders are heavily muscle-related.
Treatment may include:
- jaw exercises
- ultrasound therapy
- posture correction
- stretching protocols
- muscle rehabilitation
Physiotherapy improves jaw mobility while reducing recurrence risk.
A Multidisciplinary Advantage at FMS Dental
One of the major strengths of FMS Dental is the collaborative treatment approach involving:
- TMJ specialists
- prosthodontists
- orthodontists
- oral surgeons
- physiotherapy experts
- full-mouth rehabilitation specialists
Because severe TMD cases often involve multiple contributing factors, this multidisciplinary model allows patients to receive comprehensive care under one roof rather than fragmented symptom-based treatment.
Treatment Comparison at a Glance
| Treatment | Best For | Invasiveness | Main Benefit |
| Splint Therapy | Bruxism & mild TMD | Non-invasive | Muscle relaxation |
| TENS Therapy | Muscle pain | Non-invasive | Immediate relief |
| Low-Level Laser | Joint inflammation | Non-invasive | Reduces inflammation |
| Bite Adjustment | Bite-related TMD | Minimal | Reduces muscular overload |
| Physiotherapy | Muscle dysfunction | Non-invasive | Improves mobility |
| Orthodontics | Bite correction | Moderate | Long-term stability |
| Full Mouth Rehabilitation | Severe wear & bite collapse | Advanced | Complete bite reconstruction |
Is Surgery Ever Needed?
In most cases, no.
The majority of TMD patients improve successfully with:
- splint therapy
- muscle rehabilitation
- bite stabilization
- neuromuscular treatment
Surgery is generally reserved for:
- severe disc displacement
- advanced joint degeneration
- structural damage
- recurrent jaw dislocation
At FMS Dental, non-invasive therapies are always prioritized before surgical intervention is considered.
What Happens If TMJ Disorders Are Left Untreated?
Untreated TMD may gradually worsen over time.
| Short-Term Effects | Long-Term Effects |
| Headaches | Chronic facial pain |
| Jaw stiffness | Joint degeneration |
| Muscle fatigue | Restricted jaw movement |
| Ear symptoms | Bite collapse |
| Difficulty chewing | Sleep disturbances |
Early diagnosis almost always leads to simpler and more predictable treatment outcomes.
A Common Patient Experience
Patients seeking TMJ treatment at FMS Dental often share a similar experience:
“I thought I only had stress headaches. I never imagined my jaw and bite were the actual problem.”
After proper diagnosis and treatment, patients often report improvements in:
- headache frequency
- jaw movement
- sleep quality
- facial comfort
- chewing efficiency
Final Thoughts
TMJ disorders are far more complex than simple jaw pain. They can affect:
- headaches
- ear symptoms
- facial muscles
- neck tension
- sleep quality
- overall daily comfort
The key to successful treatment lies in identifying the root cause rather than temporarily masking symptoms.
What differentiates FMS Dental is its dedicated focus on Neuromuscular Dentistry – an advanced approach that combines digital diagnostics, muscle analysis, bite evaluation, and multidisciplinary expertise to provide comprehensive TMJ care.
Under the guidance of Dr. Faisal Zardi, patients receive personalized, evidence-based treatment designed not just for temporary symptom relief, but for long-term jaw stability, improved function, and better quality of life. If recurring headaches, jaw pain, facial discomfort, or unexplained ear symptoms have been affecting your daily life, a professional TMJ evaluation could be the first step toward lasting relief.
Frequently Asked Questions
Can TMJ problems cause headaches?
Yes. TMJ disorders can strain the muscles and nerves around the jaw, temples, and neck, often leading to recurring headaches or migraine-like symptoms.
What are the early signs of TMD?
Common early signs include jaw clicking, morning headaches, facial tightness, difficulty chewing, jaw stiffness, and teeth grinding during sleep.
Can TMJ disorders go away on their own?
Mild cases may improve temporarily, but persistent symptoms usually require professional evaluation to prevent worsening joint and muscle strain.
Is TMJ treatment painful?
Most TMJ treatments are non-invasive and focus on reducing muscle strain, improving jaw function, and relieving discomfort gradually.
What is Neuromuscular Dentistry?
Neuromuscular Dentistry looks at how the jaw joints, muscles, and bite work together to identify the underlying cause of TMJ symptoms.
When should I see a TMJ specialist?
Neuromuscular Dentistry looks at how the jaw joints, muscles, and bite work together to identify the underlying cause of TMJ symptoms.