By Prof. Dr. P. Parthasarathi Reddy, Senior Cosmetic Dentist
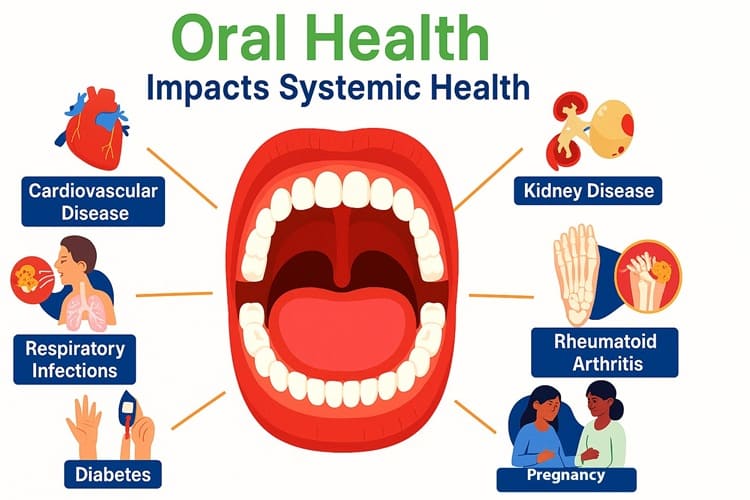
Good oral health is closely linked to your overall health. Infections like gum disease or tooth decay can let harmful bacteria enter your bloodstream, which may increase the risk of serious health problems such as heart disease, diabetes, lung infections, and complications during pregnancy. Oral health and overall health are closely connected and affect each other. Health conditions in the body can make oral problems worse, while improving oral health can also support better overall health. Practicing good oral hygiene, maintaining a healthy lifestyle and seeking regular dental and medical care are crucial for preventing and managing these interconnected health issues.
The Mouth-Body Connection
How Oral Health Impacts Systemic Health
Oral diseases like periodontitis (gum disease) are not confined to the oral cavity. The bacteria and inflammatory mediators associated with these conditions can spread through the bloodstream, influencing distant organs. Research shows that people with chronic gum disease have a significantly higher risk of systemic conditions such as diabetes and heart disease.
The Role of Bacteria and Inflammation
The mouth hosts over 700 species of bacteria, many of which are harmless or even beneficial. However, poor oral hygiene allows harmful bacteria to thrive, leading to gum inflammation (gingivitis and periodontitis). The infection triggers the immune system to release inflammatory molecules such as C-reactive protein (CRP) and interleukins (IL-6, TNF-α), which can enter the bloodstream and contribute to chronic, low-grade systemic inflammation.
This persistent inflammation is a shared risk factor in many chronic conditions, linking oral disease to systemic illness. (NIH – PMC10625740)
Oral Health and Diabetes
- Research consistently shows a two-way relationship between periodontal disease and diabetes. Chronic gum inflammation can increase insulin resistance and worsen glycemic control. In fact, people with periodontitis often have higher HbA1c levels and are more likely to develop type 2 diabetes.
- Encouragingly, studies reveal that periodontal therapy (scaling and root planing) can help reduce HbA1c levels by up to 0.4 %, improving metabolic stability.
- Clinical Insight: Managing gum disease in diabetic patients isn’t just about saving teeth but improving overall metabolic health.
Reference: MDPI Health Journal 2024 – Umbrella Review on Diabetes & Periodontal Disease
The Link between Oral Health and Cardiovascular Disease
Inflamed gums act as an entry point for oral pathogens into the bloodstream. Bacteria such as Porphyromonas gingivalis have been detected in heart valves and blockages, suggesting a role in plaque formation and arterial inflammation.
A large cohort study found that individuals with periodontal disease had a 9 % higher risk of developing coronary artery disease even after adjusting for lifestyle factors. Gum disease has also been associated with stroke, endothelial dysfunction, and increased arterial stiffness.
Did you know? Treating periodontal infections can lower systemic inflammatory markers like CRP — beneficial for heart health.
Reference: Global Heart Journal – Periodontitis & Cardiovascular Diseases Consensus Report
Oral Bacteria and Respiratory Health
Oral pathogens can be aspirated into the lungs, where they may cause or exacerbate infections such as pneumonia or worsen chronic conditions like COPD. Elderly individuals or those with poor immunity are particularly at risk.
Maintaining oral hygiene — especially in hospitalized or ventilated patients — significantly reduces the incidence of hospital-acquired pneumonia.
Reference: BMC Oral Health – Periodontal Pathogens and Respiratory Disease
Oral Health and Pregnancy Outcomes
Pregnant women with untreated gum disease face higher chances of preterm delivery, low birth weight, and gestational complications.
The mechanism? Inflammatory mediators and bacterial toxins can enter the bloodstream and disrupt placental development.
Treating gum disease before or early during pregnancy has been linked to reduced risk of adverse pregnancy outcomes.
Reference: PMC – Periodontitis and Pregnancy Outcomes
Neurological and Cognitive Health
Emerging research links oral pathogens, particularly P. gingivalis, with Alzheimer’s disease and cognitive decline. Chronic oral inflammation may accelerate neurodegeneration through systemic inflammatory and vascular pathways.
While more studies are needed, evidence suggests maintaining oral health could be a protective factor for long-term brain health.
Reference: NIH Review – Oral Bacteria and Cognitive Health
Chronic Oral Irritation and Its Link to Oral Cancer
While systemic diseases are often linked to infections and inflammation, mechanical irritation inside the mouth can also play a serious role in long-term tissue damage.
Continuous trauma from sharp or fractured tooth edges, ill-fitting dentures, or broken restorations can lead to chronic mucosal irritation — a condition that causes repeated epithelial injury, cellular turnover, and inflammation.
Over time, this persistent irritation can promote epithelial dysplasia, increasing the risk of developing oral precancerous lesions such as leukoplakia or even oral squamous cell carcinoma (OSCC), especially when combined with other risk factors like tobacco, alcohol, or poor oral hygiene.
Early recognition and removal of local irritants, along with regular oral cancer screening, are key to prevention.
Reference: Gandhi A, Khandekar S, Kannan S, et al. Chronic mechanical irritation and oral squamous cell carcinoma: A review and proposed classification. J Oral Maxillofac Pathol. 2017;21(2):330–337. DOI:10.4103/jomfp.JOMFP_55_17
How Treating Oral Disease Improves Overall Well-Being
- Reduces systemic inflammation: Scaling, root planing, and laser therapy lower CRP and IL-6 levels.
- Improves heart and metabolic health: Periodontal treatment enhances vascular function and insulin sensitivity.
- Prevents bacterial spread: Eliminating oral biofilm limits the risk of bacteremia and organ infections.
- Boosts immunity: A healthy oral microbiome supports balanced immune responses.
- Enhances quality of life: Better oral comfort, fresher breath, and improved systemic health overall.
Your mouth is the gateway to your body, taking care of it protects every system within.
🦷Practical Prevention Tips
✅ Brush twice daily using a soft-bristled brush and fluoride toothpaste.
✅ Floss or use interdental aids to clean between teeth.
✅ Rinse with an antimicrobial mouthwash if recommended.
✅ Maintain a balanced, low-sugar diet rich in antioxidants.
✅ Visit your dentist every six months for professional cleaning and early detection of gum issues.
✅ Manage stress, avoid smoking, and stay hydrated to support salivary defense.
Comprehensive Oral–Systemic Care at FMS Dental
- At FMS Dental, we believe that true oral health goes beyond your smile as it’s the foundation of your overall well-being. Every consultation begins with a comprehensive oral and systemic evaluation, where our specialists carefully assess every aspect of your dental and medical profile.
- Using advanced diagnostic tools such as digital X-rays and in-house CBCT scans, we gain a complete 3D view of your teeth, bone, and surrounding structures. A detailed medical history is reviewed, and if needed, relevant blood or diagnostic tests are prescribed to identify any underlying conditions that may affect your oral or general health.
- Our multidisciplinary team of specialists work together to eliminate all sources of oral infection, restore gum and bone health, and help you achieve a clean, stable, and infection-free mouth. Every patient receives personalized oral hygiene guidance and a maintenance plan designed to sustain long-term oral and systemic balance.
🦷 At FMS, our goal is simple: to heal, protect, and maintain the health of your mouth, because a healthy mouth means a healthier you.
⚠Disclaimer: This blog is for educational purposes only and should not replace professional dental consultation. Please consult a qualified dentist for personalized advice.
Author Bio:

Prof. Dr. P. Parthasarathi Reddy, M.D.S
Dean, Sri Sai College of Dental Surgery
Head of Department of Cosmetic Dentistry, SSCDS
Founder & Chief of FMS Dental Hospitals, India.
With over 32 years of clinical expertise, he is regarded as one of the pioneers in cosmetic and implant dentistry in South Asia. Under his leadership, FMS has grown into one of the largest private dental centers in the world.
References
- Global Heart Journal. Periodontitis and Cardiovascular Diseases: Consensus Report, 2024.
- MDPI Health Journal. Umbrella Review: Periodontal Disease and Diabetes Mellitus, 2024.
- BMC Oral Health. Impact of Periodontal Pathogens on Respiratory Diseases, 2024.
- NIH PMC. Oral Health’s Inextricable Connection to Systemic Health, 2023.
- Mayo Clinic. Gum Disease and Systemic Inflammation, 2023
Extended FAQs
How early can oral inflammation start affecting systemic health?
Even subclinical gingival inflammation (before visible gum bleeding) can raise systemic CRP levels, subtly impacting vascular and metabolic functions over time.
Can chronic oral infections affect your gut microbiome?
Yes. Oral pathogens can migrate to the gut, altering microbial balance and contributing to leaky gut syndrome, IBD, and metabolic dysfunction.
What is the “oral inflammation load,” and why does it matter?
It’s a cumulative measure of infection sites in the mouth. The more inflamed pockets you have, the higher your total systemic inflammatory burden — even if only a few teeth hurt.
Can untreated root canal infections cause systemic effects?
Yes. Chronic periapical lesions can act as persistent sources of low-grade bacteremia, potentially aggravating cardiovascular or joint conditions.
Is there a connection between gum disease and fatty liver disease?
Emerging studies link periodontitis with non-alcoholic fatty liver disease (NAFLD) through shared inflammatory and oxidative stress pathways.
How does poor oral health affect hormonal balance?
Oral inflammation can raise cortisol and pro-inflammatory cytokines, influencing hormonal regulation and worsening conditions like PCOS and thyroid imbalance.
Can dental infections worsen arthritis or joint pain?
Yes. Oral pathogens like P. gingivalis have been found in arthritic joint fluid and can trigger autoimmune responses that intensify joint inflammation.
Does treating gum disease improve kidney health?
Recent findings show that periodontal therapy can reduce markers of chronic kidney disease (CKD) and lower systemic inflammation in affected patients.
What’s the connection between oral bacteria and cancer risk?
Certain bacteria, such as Fusobacterium nucleatum, are implicated in colorectal and pancreatic cancers due to their role in chronic systemic inflammation and DNA damage.
Can oral biofilm influence chronic fatigue or brain fog?
Yes. Low-grade oral infections maintain a constant immune response that may contribute to fatigue, poor concentration, and inflammatory brain signaling.
How can CBCT scanning aid in early systemic health protection?
In-house CBCT imaging at FMS allows early detection of hidden bone infections, sinus pathologies, and impacted lesions — preventing systemic spread before symptoms appear.
Are dental metals or materials linked to systemic sensitivities?
Rarely, but metal allergies or galvanic currents can trigger localized inflammation and immune stress. Biocompatible ceramic restorations reduce this risk.
Can chronic dry mouth lead to systemic issues?
Yes. Xerostomia increases infection risk and oral acidity, indirectly worsening diabetes control and digestive imbalance due to altered saliva enzyme activity.
How do oral probiotics differ from gut probiotics?
Oral probiotics colonize the mouth and throat, balancing bacterial ecosystems locally, reducing halitosis, gingivitis, and even tonsil infections.
Can poor oral health influence fertility?
Research suggests chronic gum disease may affect sperm motility and ovulatory cycles due to systemic inflammation and immune dysregulation.
What role does vitamin D play in oral-systemic health?
Vitamin D supports immune balance, bone metabolism, and gum tissue repair. Deficiency is strongly linked to both periodontal disease and autoimmune disorders.
How does obesity link to gum disease beyond diet?
Fat cells produce TNF-α and IL-6, inflammatory molecules that worsen gum disease and amplify its systemic effects — a double inflammatory feedback loop.
Can stress-related oral issues impact systemic health?
Yes. Stress triggers bruxism, gum inflammation, and immune suppression, which increase cortisol and worsen systemic inflammatory markers.
Does oral hygiene frequency matter for systemic health?
Studies show that brushing twice daily and flossing once daily correlates with lower systemic CRP levels and reduced risk of atherosclerosis, not just cleaner teeth.
How do advanced dental lasers support systemic health?
At FMS Dental, Fotona laser therapy is used to disinfect periodontal pockets and eliminate deep-seated infection without systemic antibiotic overuse — helping reduce total body inflammation safely and effectively.