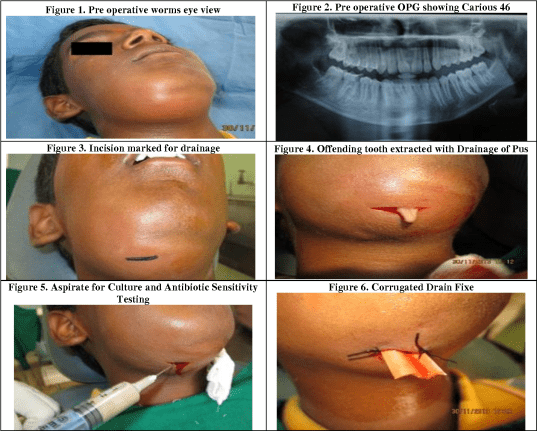
Ludwig’s angina is a form of severe diffuse cellulitis that occurs after a persistent odontogenic infection. Unless treated at an earlier stage, it could result in life-threatening situations.
It presents an acute onset and spreads rapidly, bilaterally affecting the submandibular, sublingual, and submental spaces, resulting in a state of emergency. The condition is relatively uncommon. Yet, it is potentially life-threatening due to the risk of impending airway obstruction. Taking into account its invasive nature and aggressiveness, early identification and management of Ludwig’s angina are extremely important. Early addressing and proper management with appropriate treatment planning could be a life-saving procedure.