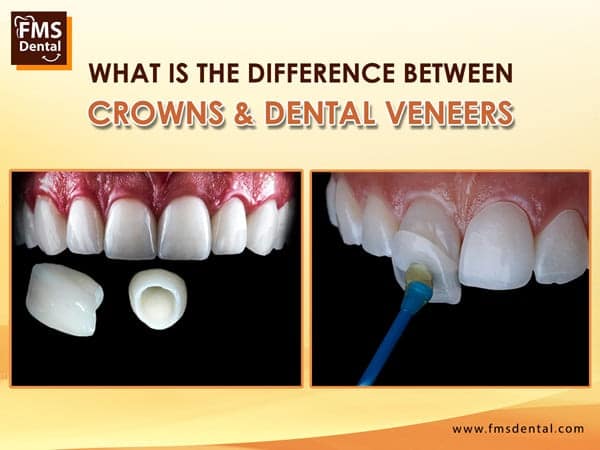
How to Prepare for Oral Surgery/minor surgeries?
Oral surgery can go a lot easier if you put in a little preparation. If you know what to expect ahead of time, you may be more at ease about what you need to have done. Your process should start long before you walk in for your appointment.